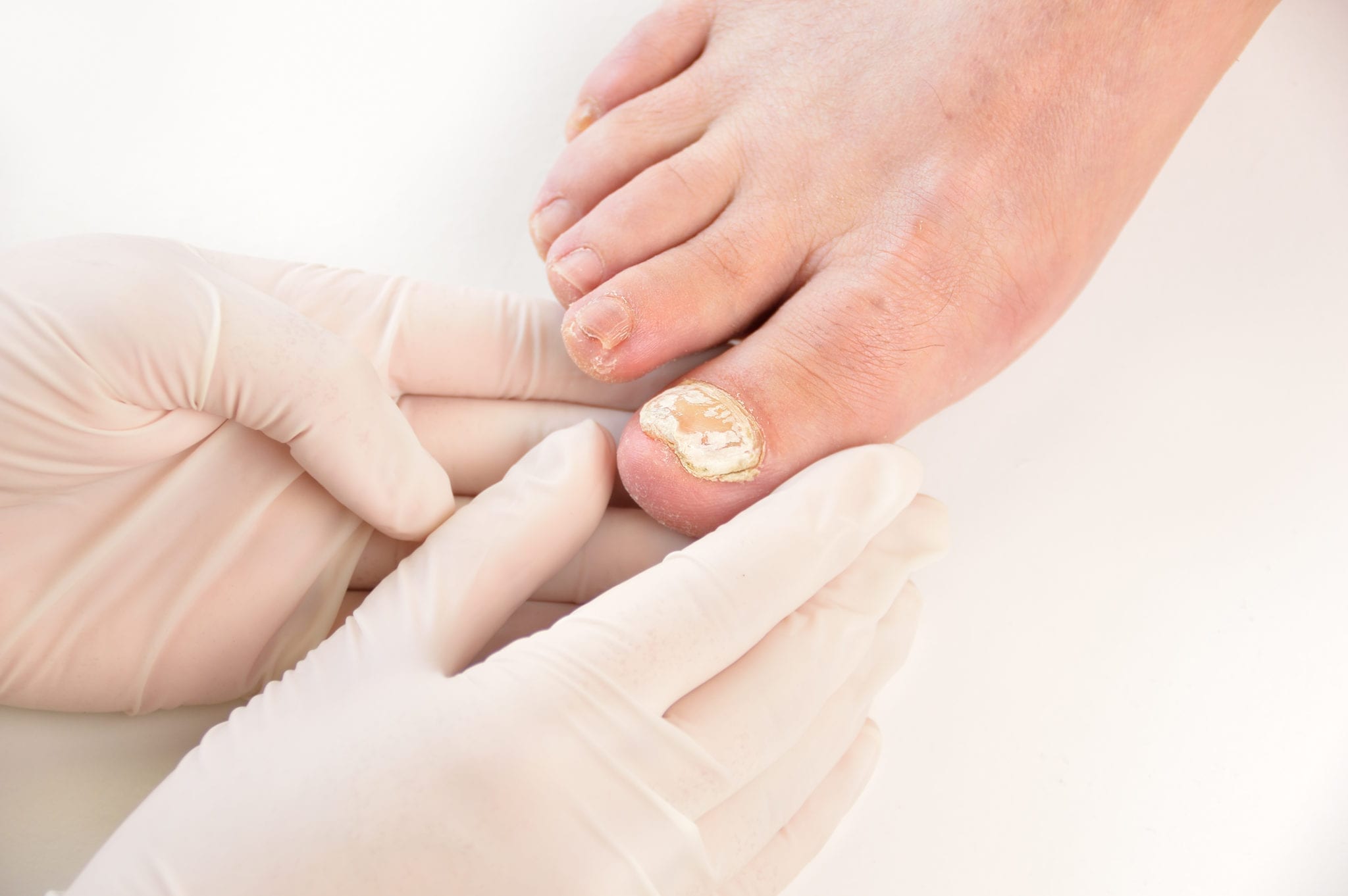
Why Toenail Fungus Is So Hard to Get Rid Of
Toenail fungus, medically known as onychomycosis, develops when microscopic fungi begin growing beneath the nail plate in the nail bed. Because the infection lives under the nail rather than on the surface, it can be difficult to detect early and even harder to eliminate once established. Over time, the fungus disrupts normal nail growth, causing discoloration, thickening, brittleness, and sometimes separation from the nail bed.
Fungal organisms thrive in warm, dark, and moist environments. For this reason, sweaty feet trapped inside closed-toe shoes create ideal conditions for infection. Locker rooms, gyms, and communal showers also increase exposure risk. Although anyone can develop toenail fungus at any age, it becomes more common with advancing age, particularly in individuals over 65. Toenails are affected more frequently than fingernails because they grow more slowly and spend more time confined in shoes.
One of the biggest reasons toenail fungus is so difficult to treat is a common misconception about where the infection lives. Many people assume the fungus sits on the surface of the nail. As a result, they rely solely on topical treatments that may not penetrate deeply enough to reach the infected nail bed. In reality, dermatophytes, the microscopic fungi responsible for most cases, embed themselves under the infected nails, where they remain protected and can continue to thrive.
Understanding how toenail fungus develops and why it persists is the first step toward choosing an effective treatment strategy.
Why Toenail Fungus Often Persists Despite Treatment
Toenail fungus rarely resolves on its own. If you have not pursued any form of treatment, that is typically the first step. Because the infection lives beneath the nail plate, it remains protected and continues to grow unless actively addressed.
Many individuals initially try home remedies such as menthol-based ointments, essential oils, or other over-the-counter products. While these approaches may improve the nail’s appearance temporarily, they often fail to reach the underlying infection in the nail bed. As a result, the fungus may continue to persist despite months of at-home care.
Even when patients seek medical treatment, outcomes can vary. Not all therapies offer the same level of effectiveness, and the severity of the infection plays a major role in treatment success.
Common Treatment Options
Topical Medications- Prescription topical antifungal treatments are often recommended for mild cases. However, thickened or hardened nails can limit penetration, making it difficult for the medication to reach the source of the infection. These treatments typically require daily application for many months before noticeable improvement occurs.
Oral Antifungal Medications- Oral antifungal medications work systemically, meaning they travel through the bloodstream to reach the nail bed from within. They generally provide higher cure rates than topical treatments. However, they require several weeks to months of use, and healthcare providers may monitor liver function during treatment to ensure safety. Not all patients are ideal candidates for oral therapy, particularly those with certain underlying health conditions.
Because treatment success depends on infection severity, nail thickness, overall health, and consistency, some individuals may need to explore alternative or combination approaches if initial therapies do not produce desired results.
Laser Treatment for Nail Fungus
Laser therapy has become an increasingly popular option for treating toenail fungus, particularly for patients who have not responded to topical or oral medications. The FDA-cleared PinPointe™ laser uses focused light energy to penetrate the nail plate and target fungal organisms beneath the surface.
Unlike topical treatments, which must pass through thickened nail tissue to reach the infection, laser energy travels directly through the nail to the affected area. Additionally, because laser therapy does not circulate through the bloodstream, it avoids the systemic concerns sometimes associated with oral antifungal medications, such as medication interactions or liver monitoring.
Treatment sessions are typically brief and performed in the office. Most patients describe the sensation as mild warmth, and there is no required downtime afterward. While some individuals may see improvement after a single session, outcomes vary depending on the severity of the infection and the thickness of the nail. In certain cases, additional treatments may be recommended.
As with all treatment options, visible improvement depends on healthy nail regrowth, which can take several months.
What Happens After Treatment? Preventing Recurrence
Many patients feel relieved once their toenail fungus appears to clear. However, recurrence is common if preventive steps are not maintained. Because fungal spores are widespread in the environment, reinfection can occur months after treatment, sometimes presenting with the same discoloration and thickening as before.
Recurrent toenail fungus can feel discouraging, especially for individuals who have previously tried creams, oral medications, or other therapies. However, recurrence does not necessarily mean treatment failed. Often, it indicates that fungal exposure continued or that preventive measures were insufficient.
Long-term success depends not only on eliminating the active infection but also on maintaining proper foot hygiene, disinfecting footwear, and addressing risk factors such as moisture buildup or nail trauma.
With the right treatment plan and consistent preventive care, the likelihood of recurrence can be significantly reduced.
Why Toenail Fungus Comes Back and How to Prevent It
Toenail fungus has a frustrating tendency to come back, even after an effective treatment. In many cases, recurrence happens not because treatment failed, but because underlying risk factors were never fully addressed.
One common reason for recurrence is incomplete treatment. Many over-the-counter products only treat the surface of the nail. However, the infection typically lives under the nails in the nail bed. If the fungus is not fully eliminated at its source, it can quietly persist and regrow over time.
Another major factor is forgetting aftercare. Even after successful treatment, returning to old habits, such as failing to disinfect footwear or walking barefoot in locker rooms, can reintroduce fungal spores. Because these organisms thrive in warm, moist environments, shoes, gym floors, nail salons, and communal showers remain common sources of exposure.
Additionally, nails that have previously been infected may become structurally weakened. Damage from prior infection can make the nail more vulnerable to reinfection, especially if preventive measures are not maintained.
Reducing recurrence requires a proactive approach. Key preventive steps include:
- Choosing an effective treatment plan appropriate for the severity of the infection
- Disinfecting shoes regularly with antifungal sprays or UV sanitizers
- Keeping feet clean and dry
- Changing socks daily and rotating shoes
- Wearing protective footwear in public showers and locker rooms
- Ensuring proper sterilization at nail salons or bringing personal tools
- Using preventive antifungal powders or sprays when needed
Long-term success depends on combining proper treatment with consistent prevention. By addressing both the infection and the environmental risk factors, you can significantly reduce the likelihood of toenail fungus returning.
Why Patients Trust Laser Nail Therapy
At Laser Nail Therapy, we focus on long-term results, rather than just a quick fix. Our laser treatment not only clears the infection but also significantly lowers the chances of reinfection.
We utilize the PinPointe™ FootLaser®, the leading FDA-cleared laser for treating nail fungus. It’s painless, requires no recovery time, and is designed to destroy the fungus at the source: beneath the nail surface. This allows for results that last.